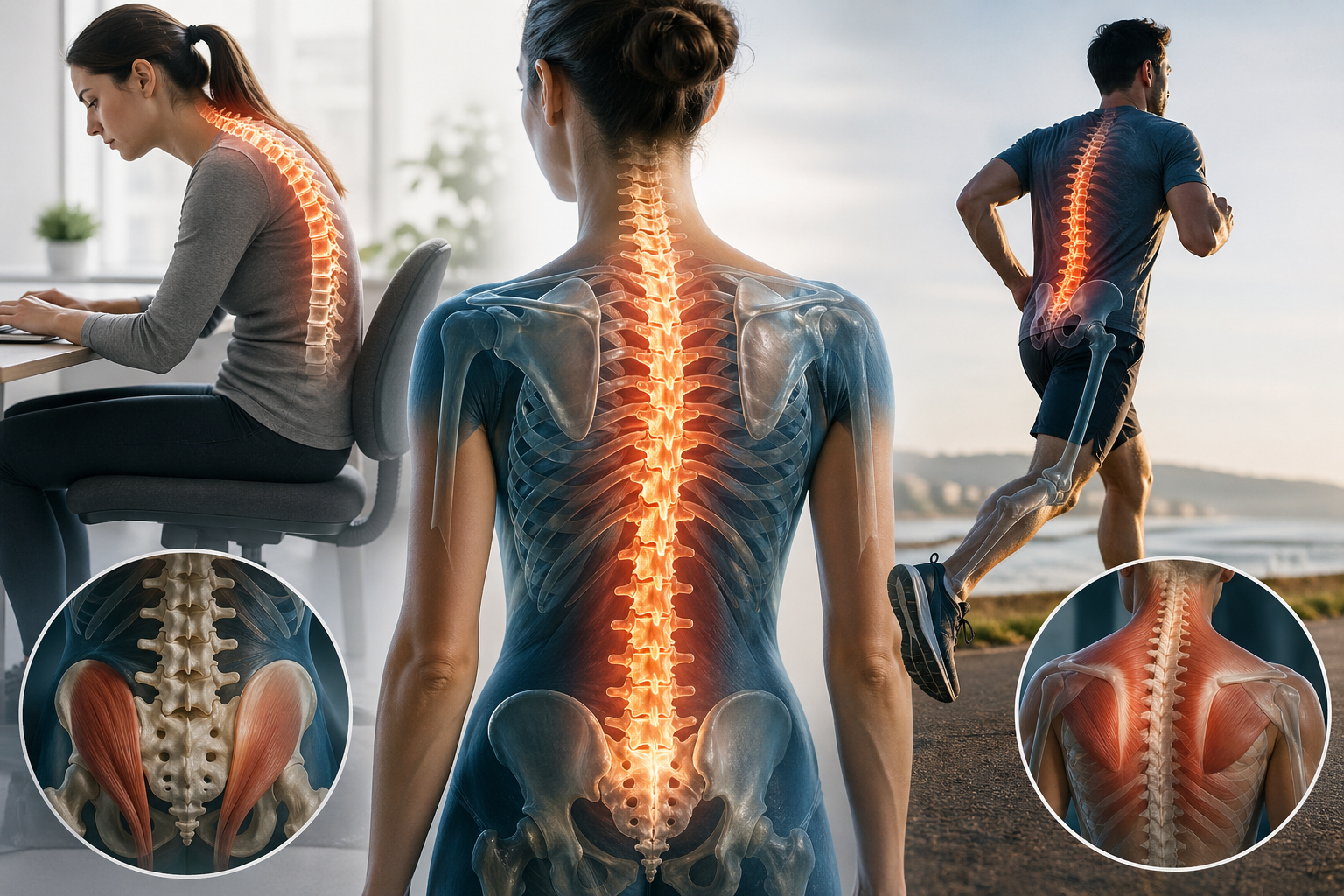
Understanding Biomechanics: How Posture, Gait, and Muscle Imbalances Affect the Spine
Most people don't think about their spine until something hurts. But long before pain appears, changes in how you hold yourself, walk, and use your muscles are quietly loading your spine in ways it was not designed to handle. Research published in the Journal of Orthopaedic and Sports Physical Therapy has found that altered movement patterns are a significant contributor to musculoskeletal pain, and many of those patterns go undetected for years.
Understanding spinal biomechanics and how forces move through your spine during everyday activity is one of the most practical tools for both preventing injury and recovering from it. Whether you sit at a desk all day, spend hours on your feet, or stay active with sports and recreation, what your body does moment to moment shapes the long-term health of your spine.
What Is Biomechanics? And Why Does It Matter for Your Spine?
Biomechanics is the study of how mechanical forces act on living structures. In the context of spinal health, it describes how your muscles, joints, and connective tissues work together to support and move your body. When everything is functioning well, the spine distributes load efficiently across its vertebrae, discs, and surrounding muscles.
The problem starts when something in that system is off.
Your spine has three natural curves: cervical (neck), thoracic (mid-back), and lumbar (lower back). Each curve plays a specific mechanical role. When posture, gait, or muscle balance disrupts those curves, stress accumulates in ways the spine is not built to manage over time. That stress can lead to disc compression and degeneration, facet joint irritation, muscle fatigue and compensatory tightness, nerve root irritation, and chronic postural strain.
This is not abstract science. It is the reason a person with perfect MRI results still has pain, or why someone else with disc changes feels completely fine. Structure matters, but how you use and load that structure matters just as much.
Posture, Gait, and Movement Patterns: What Is Actually Happening to Your Spine
Posture and Spinal Load
Posture is not just how you look standing in a mirror. It is how your spine distributes gravitational force at rest and in motion. When your head shifts forward, a pattern often called forward head posture, the effective weight your cervical spine must support increases significantly. A head that sits two inches in front of neutral can more than double the mechanical load on the neck and upper back.
The same principle applies to the lower back. Excessive lumbar extension, flattening of the natural curve, or a forward pelvic tilt all shift load onto structures that are not built to handle it long-term. Over time, these postural patterns contribute to disc wear, muscle imbalance, and persistent discomfort.
Gait and Movement Patterns
How you walk tells a skilled clinician a great deal about what is happening throughout your entire musculoskeletal system. Healthy gait is a coordinated rhythm where hip extension, arm swing, trunk rotation, and foot contact all work together to absorb and transfer force efficiently.
When any part of that system breaks down, the spine compensates. Common gait issues that affect spinal health include reduced hip extension, which forces the lumbar spine to pick up the movement slack; overpronation or excessive inward rolling of the foot, which shifts force up through the knee and into the pelvis and lower back; asymmetrical arm swing, which is often a sign of rotational restrictions in the thoracic spine; and shortened stride length, which limits the hip mobility needed to offload spinal structures during movement.
These patterns do not always cause immediate pain, but they create the mechanical conditions for strain, degeneration, and injury over time.
Muscle Imbalances Explained: Why Strength Alone Is Not Enough
Muscle imbalances occur when certain muscles become overactive and tight while opposing muscles become underactive and weak. This is not about overall fitness. Highly active people develop significant imbalances depending on the demands of their sport or occupation.
Common imbalance patterns that affect the spine include tight hip flexors combined with weak glutes, which creates anterior pelvic tilt and increases lumbar lordosis, overloading the lower back. Weak deep cervical flexors paired with tight suboccipitals contributes to forward head posture and chronic neck tension. Inhibited lower trapezius combined with an overactive upper trapezius disrupts shoulder mechanics and loads the cervical spine. Tight thoracic paraspinals with poor thoracic mobility restricts rotation and forces the lumbar spine to compensate.
These patterns are often reinforced by repetitive activity, whether sitting in the same position, performing the same athletic movements, or favoring one side of the body. Without targeted assessment and correction, they tend to worsen gradually.
Structural vs. Inflammatory Conditions: Knowing the Difference
Not all spinal pain has the same origin. Understanding the distinction helps guide appropriate care.
Structural or mechanical conditions such as disc herniation, facet syndrome, and postural strain are typically driven by how forces move through the spine. They often worsen with sustained positions or specific movements, and improve with movement, positional changes, or targeted manual therapy.
Inflammatory conditions such as ankylosing spondylitis or rheumatoid arthritis affecting the spine involve immune-driven joint inflammation and often follow different patterns: stiffness that is worse in the morning, improvement with movement, and symptom behavior that does not follow typical mechanical patterns.
This distinction matters because the approach to care differs. Biomechanically driven pain responds well to movement correction, manual therapy, and functional rehabilitation. Inflammatory conditions typically require co-management with appropriate medical providers.
If your symptoms include significant morning stiffness lasting more than 45 minutes, unexplained systemic symptoms, or pain that does not respond to typical mechanical interventions, a broader clinical evaluation is warranted.
When Is Imaging Necessary?
Imaging such as X-ray, MRI, or CT is a useful tool, but it is not always the first or most informative step. Research consistently shows that many people with significant findings on imaging including disc bulges, degeneration, and osteophytes have no pain at all, while many people in significant pain show minimal imaging abnormalities.
Imaging becomes more important when neurological signs are present such as weakness, numbness, or bowel and bladder changes; when symptoms follow significant trauma; when red flags suggest a non-mechanical cause such as fever, unexplained weight loss, or a history of cancer; or when conservative care has not produced expected improvement within a reasonable timeframe.
For most people with postural pain, movement-related discomfort, or suspected muscle imbalance patterns, a functional clinical assessment that evaluates how you actually move provides more actionable information than imaging alone. That is where biomechanical evaluation becomes essential.
Assessment Options in Grand Haven: Where to Start
If you are dealing with persistent back or neck pain, recurring muscle tension, or movement patterns you suspect are not quite right, a functional assessment is the logical starting point.
At Movement Chiropractic Center in Grand Haven, Dr. Hailey Watkins takes a whole-body approach to understanding how your structure, movement, and muscle function are connected. With a background in kinesiology, the formal study of human movement, and additional training working with athletes, pregnant mothers, and active patients, Dr. Watkins is equipped to evaluate the biomechanical patterns that often sit beneath the surface of chronic pain.
Two services particularly relevant to spinal biomechanics are functional muscle testing in Grand Haven, which identifies inhibited or overactive muscle patterns contributing to imbalance and spinal strain, and trigger point therapy for muscle pain, which addresses myofascial tension patterns that maintain mechanical dysfunction and restrict healthy movement.
Movement Chiropractic Center serves Grand Haven and the surrounding West Michigan lakeshore community at 849 Park Avenue, Suite 200, Grand Haven, MI.
What Patients Are Saying
"Best adjustment I've had in 20 years. Good muscle work mixed in, too. Highly recommend." — Luke H., Google Review
"Great with kids! Friendly and inviting. Respectful and informative. Effective, thorough, and professional. 10/10 would highly recommend." — Ried M., Google Review
"Excellent experience! Dr. Hailey is very thorough." — D.B. Cooper, Google Review
Ready to Understand What Your Body Is Telling You?
Chronic pain, recurring tension, and movement that does not feel right rarely resolve on their own, especially when the underlying biomechanical patterns have not been identified.
If you are in Grand Haven or the West Michigan area and want to understand what is actually happening in your spine, Movement Chiropractic Center is ready to help. Dr. Hailey Watkins offers individualized, movement-based care grounded in a genuine understanding of how your body works.
Schedule your appointment today and take the first step toward moving better and feeling your best.
849 Park Avenue, Suite 200, Grand Haven, MI 49417 Phone: 616-402-5994